What is Deep Vein Thrombosis?
Deep venous thrombosis (DVT) is a condition that occurs when a blood clot, or thrombus, forms in a major vein, usually in the leg. The clot can partially or completely block off the blood flow through that vein.
Veins are the vessels that return the blood to the heart, so a blockage of that circulation can lead to poor emptying of blood in the extremity, causing swelling and pain. If the clot is not treated, all or part of it can break off and travel up to the heart, through it, and into the lungs. In the lungs, it can obstruct blood supply with life-threatening consequences. This is known as a pulmonary embolism (PE). If you’re experiencing possible symptoms of venous insufficiency or DVT, GO IMMEDIATELY TO YOUR CLOSEST EMERGENCY ROOM. Knowledge is power, and, in this case, can be lifesaving.
Vein Treatments at Wisconsin Vein Center & MediSpa
1. Endovenous Laser Treatment
2.Ambulatory Phlebectomy Treatment
3. Varithena Varicose Vein Treatment
4. Spider Vein Treatment
5. Compression Hose

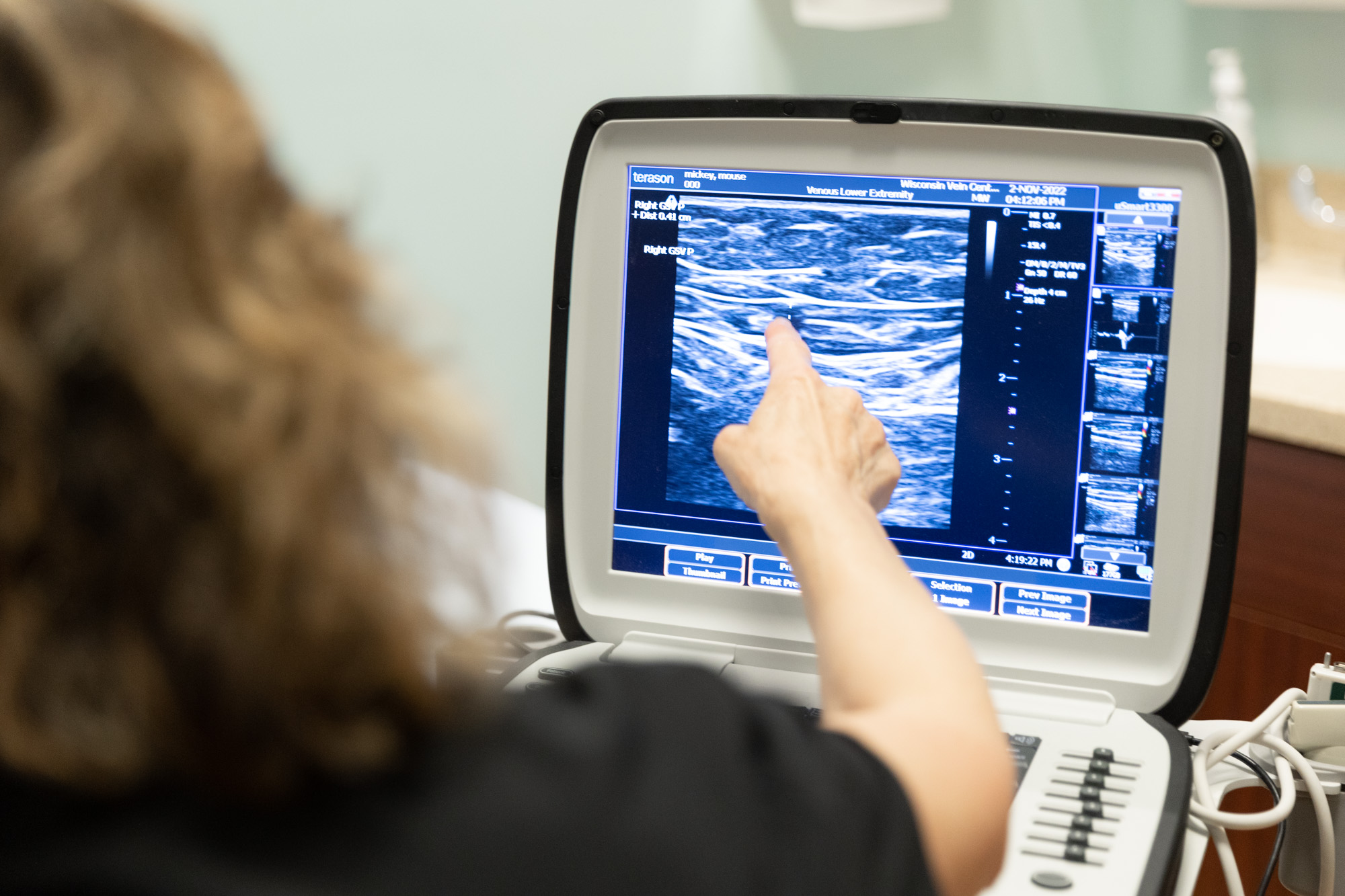

More Information About DVT
Massive pulmonary embolism attributed to DVT causes over 300,000 deaths in the United States each year. That’s more than deaths from breast cancer and HIV disease combined. PE is the leading cause of preventable in-hospital mortality.
There are certain people who are more at risk than others to develop DVT. Age plays a major role. Although a blood clot can develop in anyone, the older you are, the greater the likelihood. Additional risk factors include immobilization due to hospitalization, recent surgery, pregnancy and the first weeks postpartum, and long air or car trips.
Other conditions which are known to have a higher risk include cancer, stroke, heart failure, and varicose veins. Injuries such as lower extremity fractures can also cause blood clots to form. Finally, there are conditions that make the blood more likely to coagulate or clot. These include certain blood disorders that may be inherited and medications such as birth control pills or estrogens. The more risk factors an individual has, the more likely he or she is to develop DVT.
DVT does not always cause symptoms. But larger clots can lead to leg pain and swelling. DVT is a serious problem that requires immediate medical attention. Blood thinners are usually needed, and clot-busting medication may be indicated. If left untreated, a fatal PE can occur, or permanent venous insufficiency can lead to chronic leg swelling and ulceration.
DVT Prevention Tips
The most important thing you can do to help prevent DVT is to keep your body moving. If you are in a hospital or sitting for several hours in a car or plane, you must exercise. If you cannot get up and walk, then you should exercise in such a way that you can keep the blood moving in your legs.
Some DVT prevention tips to remember when traveling or when sitting for extended periods of time include:
- Avoid crossing the legs at the ankles or knees and regularly change leg position.
- Stay hydrated, drinking nondiuertic beverages such as water, milk, and juice.
- Exercise at least every hour on long journeys or when sitting for a long period of time.
- Wear loose-fitting clothing when flying. Parts of your body can expand because of atmospheric pressure in a plane.
- Wear graduated-compression stockings when flying.
Varicose Veins & DVT
People with varicose veins are at a higher risk of developing DVT. Why is this the case? Varicose veins are superficial veins. They are not the veins we talk about when we are describing deep venous thrombosis, but they do connect to the deep veins.
Varicose veins are larger and more twisted than normally functioning veins, so they are even more likely to develop a clot. The blood moves more slowly through the varicose vein than through a nice straight vein. Immobility, or sitting in a cramped position for a prolonged period, slows the blood flow down even more, making clots more likely. This condition is called superficial phlebitis.
Because the varicose vein is so abnormal, the clot can propagate, or grow larger, and up the vein toward the deep vein system. If the clot extends to the deep vein, or if some breaks off and gets into the deep vein, a pulmonary embolus can occur.
To help prevent phlebitis and DVT, people with varicose veins should always do leg and foot exercises and wear graduated compression hose or stockings when they sit still for any prolonged period of time, even at work in an office.


about
Why Choose Wisconsin Vein Center & MediSpa?
Wisconsin Vein Center & MediSpa is a physician-owned and operated facility. At the core of our practice is a dedication to providing the most effective treatments and products available to create results patients can be proud of.
With a state-of-the-art facility, advanced treatments, and an experienced team of experts, our med spa in Greater Milwaukee provides the highest standard of care.
Just minutes away from Milwaukee and Waukesha, our facility provides the comfort of a relaxed spa environment designed for women and men of all ages. We focus on enhancing your wellness and beauty, with the additional benefit of an on-site physician in order to offer more advanced treatments and procedures than a traditional spa.
Learn More

Have Questions? We’re Here to Help.
Wisconsin Vein Center & MediSpa is committed to helping patients live healthy lives free of limitations. If you have questions or concerns about your vein health, contact us today or schedule an appointment with one of our expert clinicians.